Damaged skin: 3 types of lesions
1/ Ecchymosis
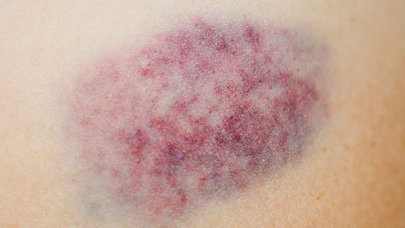
An ecchymosis occurs when small blood vessels in the skin rupture after an impact. Blood and red blood cells accumulate in neighbouring tissues and form a visible coloured spot on the skin’s surface. This bruise is often painful to the touch; the harder the knock, the more painful it is. The colour of an ecchymosis changes over time as the haemoglobin in the red blood cells is resorbed into the skin. The ecchymosis starts out red, then becomes black, blue and finally, green. At the end of the capillary repair process, it is yellow/brown and remains that colour for one to two weeks. But it can take longer if the lesion is large. The different colours correspond to the various stages the haemoglobin accumulated in the skin goes through as it breaks down.
2/ Oedema
An oedema — also called a bump — occurs when the skin swells at the place of impact. It can appear rapidly after the knock. It is triggered by a blood plasma effusion in the neighbouring tissues. Plasma is the fluid in which the red blood cells circulate inside the blood vessels.
3/ Haematoma
A haematoma is the combination of an ecchymosis (bruise) and an oedema (bump). The first thing you should do is to apply compression and ice to the area impacted or to speed up elimination with targeted active ingredients before seeing a doctor, if necessary.