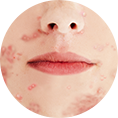
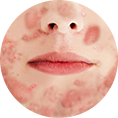
Understand my skin
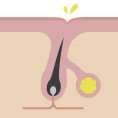
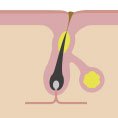
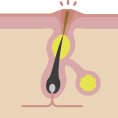
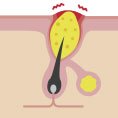
Why do I have acne and how to treat it?
Acne isn’t necessarily a severe skin condition, but it has a huge impact on self-image and quality of life. It needs to be taken care of, especially if you’re feeling depressed, angry or helpless. To win the blemish battle once and for all, it’s important to know why we have pimples and how acne works. Let’s get under your skin.